Case
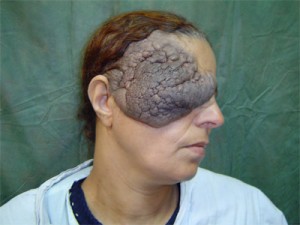
This is a case about John, a 26-year-old man, who has Neurofibromatosis, also known as elephant man’s disease, a neurological disease in which non-malignant tumors attach to the body’s nerves. This disease causes severe disfigurement and radical impairment of bodily functions. John was first diagnosed when he was 7-years-old and in the last 20 years, he has had over 100 surgeries to try to remove the tumors. These surgeries have had severe side effects resulting in John being deaf, partially blind, almost entirely paralyzed, and in need of a respirator to keep breathing. The medical professionals that have been caring for him say that there is no chance of remission. Based on his past experience, John has requested to not have anymore surgeries and for the medical professionals disconnect him from the respirator, which will inevitably cause his death. His family initially strongly disagrees with John but is ultimately convinced to support him. The medical team says that he would be able to live for years on the respirator but they too are prepared to disconnect it (Tomas and Wilfrid 209).
Dilemma
In this case the doctors face a dilemma between nonmaleficence and respect for autonomy. They have previously been acting under the principles of autonomy and beneficence because John had given consent to his previous surgeries and the acts that were taken were done so to save his life. The situation has changed and now beneficence has turned into a question of nonmaleficence.
Discussion
I argue that the doctors ought to disconnect the respirator and allow John to die. Nonmaleficence is in question because if they unplug the respirator they are technically doing an act that will cause harm because they are aware that John’s body cannot sustain his life alone. Since John has changed his mind about what he consents to, the doctors now have to balance between their respect for his autonomy and their value of doing no harm. The basis of autonomy starts with John’s competence. The doctors have described him as “fully alert, conscious, and in control of his mental faculties” (Tomas and Wilfrid 209). That description proves that John is considered a competent patient. The doctors ought not to question John’s competence when he expressed his wishes to allow his disease to take his life. He has shown a full understanding of his situation. He is aware that he has had countless surgeries yet he is not improving. This case also calls one to look at the distinction between killing and letting die. These doctors are technically killing John because they are taking an action that will result in his life ending but it is not that clear. This case blurs the lines between killing and letting die. Once the doctors take that action they are letting him die because once he is unable to breath they will intentionally not put him back on a respirator. Beauchamp and Childress state that part of letting one die is that “disease, system failure, or injury causes death” (Beauchamp and Childress 175). I argue that John’s brain disease will ultimately end his life, not the doctors. The medical team also does not feel comfortable with giving him a strong enough dose of medication that will accelerate his death. They are morally correct in this because that would enter the realm of killing rather than letting him die. Beauchamp and Childress go on to state that it is acceptable to let one die if the “medical technology is useless… or patients or their authorized surrogates validly refused a medical technology” (Beauchamp and Childress 175-176). In John’s case both of these conditions are met. The medical technology, surgeries and a respirator, have not been successful in treating him rather they have just kept him alive and, as stated above, he has now refused the technology. McIntyre gives further support of the moral acceptability for a physician to withdraw a life sustaining treatment because he is doing it “only to respect his patient’s wishes and ‘to cease doing useless and futile or degrading things to the patient when [the patient] no longer stands to benefit from them” (McIntyre 62). Nonmaleficence can be further specified in this case as do no harm except if the patient is competently refusing medical treatment and has no real hope for improvement. The medical team ought to disconnect the respirator and is morally justified in doing so.
References
Beauchamp, Tom L., James F. Childress. Principles of Biomedical Ethics. 7th ed. N.p.: Oxford University Press, 2012. Print.
Thomas, John E., and Wilfrid J. Waluchow. Well and Good: A Case Study Approach to Health Care Ethics. 4th ed. Toronto: Broadview, 2014. Print.
Picture
http://geneticdisorders247.wikispaces.com/Neurofibromatosis