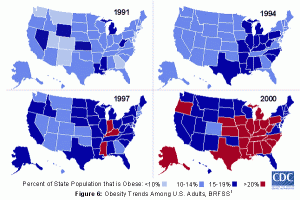
Obesity Trends
Most Emory students who have taken a health or global health class have seen the CDC video of the staggering obesity trends in the US. If not, you must see it. 30 years ago, the highest rates of state-wide obesity were at 14 percent. Now, in the 2000’s, 14% is an incredibly low, unheard-of percentage of obesity. The rates of obesity currently exceed 30% for some states. Although debatable, obesity is considered an epidemic. When evaluating these CDC statistics, it’s easier to develop a stronger argument for obesity interventions in our country.
Hard Paternalism, Soft Paternalism, Maternalism
Holm asks “When can paternalism be justified?” The obesity rates in America have gotten out of hand. We are trying to combat the obesity trend with a larger focus on exercise and health (in grade schools, college, workplace, gyms, grocery stores, social media, etc.), remodeling the food pyramid, offering programs like weight watchers, etc. However, these are mostly voluntary interventions, and none of these interventions are coercive. As a country, it is difficult to impose mandatory interventions or any measures that represent the hard paternalism that Holm describes. On the other hand, we already use soft paternalism as a means to intervene in obese families; similar to the example of telling a smoker that if you smoke, you die, you can tell a mother that if you feed the child an unhealthy diet he will become obese and develop dangerous health problems. Furthermore, to soften the intervention and its accompanying statements, we can add maternalism to soft paternalism. For example, just like telling a mother that drinking alcohol during pregnancy can be potentially harmful, we can tell a parent that feeding their child an unhealthy diet can potentially harm the child, leading to preventable diseases like obesity and diabetes. Doctors use their social skills to talk to the parents of an overweight or obese child without sounding too offensive. Arguably, hard paternalism is too harsh, and maternalism may prove ineffective. Soft paternalism, whether or not used in combination with maternalism, is an effective way to introduce a need for intervention. This should most likely represent an intervention from a doctor (a pediatrician probably), or a different professional, such as a dietician.
Should Cost be a Factor?
Additionally, obesity contributes to America’s rising health costs. The CDC states that “in 2008 dollars, these [obesity] costs totaled about $147 billion.” Since then, obesity rates have not improved, and the cost has remained astonishingly high. Holm argues that we should not intervene with people’s lives and their comfortable lifestyles for the sake of money, but this is just the tip of the iceberg. The high costs associate with obesity are only a symptom of the problematic matter at hand. The statistics outlining obesity-related costs beg for attention- in this case, money can be used as a motivational factor for obesity interventions. Holm also states that “pure economic gain is usually not considered sufficient reason to claim that the common good is being promoted,” but this money comes from our tax dollars, and every person that pays taxes or utilizes the health system in the United States is affected by high healthcare prices. Although intervening would not result in economic gains, it will result in economic relief, since the strain of obesity on our healthcare system will loosen.
Conclusion
I agree that imposing interventions on obese children is paternalistic. However, if the kid is obese, the parents are probably obese, and their parents are probably obese too. The cycle of abuse has to stop somewhere. Intervening while a child is young can possibly break this vicious cycle. By employing well-phrased, maternalistic/ soft-paternalistic discussion, we can introduce interventions in a non-coercive way and possibly reverse some of the shocking trends we see in Obesity trends in the US.
Centers for Disease Control and Prevention. (2012). What Causes Overweight and Obesity? Retrieved from: http://www.cdc.gov/obesity/adult/causes/index.html
Holm, S. “Obesity Interventions and Ethics.” Arguing About Bioethics. Ed. Stephen Holland. London: Routledge, 2012. 392-97. Print.