Case:
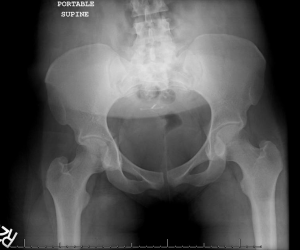
A young person presented following an MVC. Initial workup was negative including plain films of the chest and pelvis, however the patient had some tenderness over the right greater trochanter, and some pain with passive ROM, limiting movement overall. On tertiary exam in the ED, the patient was unable to bear weight on the right leg on multiple attempts, even after morphine administration.
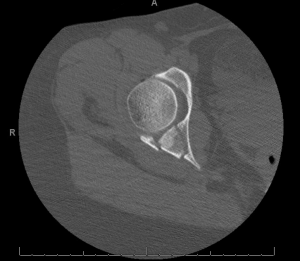
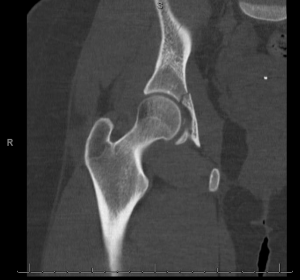
CT of the hip was obtained which showed a comminuted fracture through the posterior acetabular wall.
This patient has an occult hip fracture.
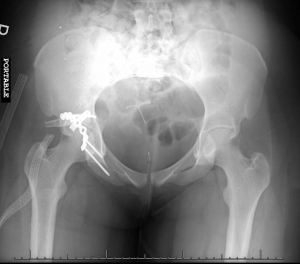
The patient was admitted to orthopedics and taken to the OR for operative repair.
Imaging the Hip:
- Plain radiographs have a sensitivity between 90-98% for hip fracture
- Prevalence of occult hip fracture is 3-4% (some say as high as 9%)
- CT is good, but not the best – 58-70% sensitivity for occult fracture
- MRI has 100% sensitivity, and is considered the gold standard
Characteristics of Patients with Occult Hip Fractures:
- Inability to bear weight – most common finding
- Pain with axial loading of hip (useful in non-ambulatory patients i.e. nursing home)
- Extremity held in internal/external rotation
- Consistent history (fall, trauma, etc)
- Marked change from pre-fracture mobility
Bottom Line:
Occult fractures exist, and missing these injuries have both high morbidity, and missed orthopedic injuries are the most frequent cause of litigation against Emergency Physicians3. Based on availability, CT is probably the “next best test” for patients with high clinical suspicion of a fracture, however even with a negative CT, you may need to admit for MRI.
References:
- https://www.ncbi.nlm.nih.gov/books/NBK83026/
- ACR Appropriateness Criteria Suspected Hip Fracture
- Orthopedic pitfalls in the ED: radiographically occult hip fracture.

1 comments
Good case. I’ve had a couple of these. It’s a great reminder to know your study’s limitations and that clinical reassessment of the patient rules.