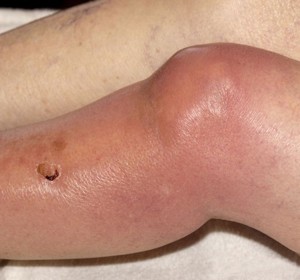
Clinical Question: What would you do if you have a patient with cellulitis, but you are still worried about an underlying septic joint??
Clinical Vignette: 47 yo M with L knee pain, swelling, redness and immobile. PE: Fever, tachycardia, and a swollen L knee
- Phys Ex:
- Clinically cannot move the joint
- Source
- Staph is most common pathogen (80-90%)
- N.gonorrhea account for the rest in the general populous but it is typically polyarticular
- Dx: (different studies have variant findings, but these are collated from a few cited below)
- WBC and PMNs – different studies show different cut offs
- WBC counts
- <25,000/microL: LR, 0.32
- > or =25,000/microL: LR, 2.9
- >50,000/microL: LR, 7.7
- PMNs
- > 90%: LR of 3.4
- <90%: LR, 0.34
- WBC counts
- Synovial Lactic acid with a cut off value of <4.3 is highly unlikely to be septic arthritis, while >10 is highly probable
- ESR/CRP – not consistent across trials with no cut off that significantly increases or decreases post test probability for septic arthritis
- One Study by Li
- ESR > 30: sensitivity of 96%
- ESR > 20: sensitivity of 75% and specificity of 11%
- One Study by Ernst
- ESR > 15: Sensitivity of 66%
- CRP > 0.8: Sensitivity of 90%
- One Study by Li
- WBC and PMNs – different studies show different cut offs
- Tx:
- G+ : coverage for MRSA: Vancomycin
- G- bacilli: cover pseudomonas: Ceftriaxone 2g IV once daily
- Gram indeterminate – treat with vancomycin in immunocompetent patients and vancomycin + 3rd generation cephalosporin in immunocompromised patient, IVDU, or traumatic bacterial arthritis
At Grady, the Orthopedic service would like an ESR, CRP, Gram stain and culture, along with a sample of the synovial fluid for them to view after the joint is tapped when evaluating for septic arthritis.
If you have an overlying cellulitis but are still concerned for a septic joint, what do you do?
Lenski, Markus, and Michael A. Scherer. “Analysis of Synovial Inflammatory Markers to Differ Infectious from Gouty Arthritis.” Clinical Biochemistry 47.1-2 (2014): 49-55. Web.
Margaretten, M. E., J. Kohlwes, D. Moore, and S. Bent. “Does This Adult Patient Have Septic Arthritis?” JAMA: The Journal of the American Medical Association 297.13 (2007): 1478-488. Web.
Carpenter, Christopher R., Jeremiah D. Schuur, Worth W. Everett, and Jesse M. Pines. “Evidence-based Diagnostics: Adult Septic Arthritis.”Academic Emergency Medicine 18.8 (2011): 781-96. Web.
Li, S. F., C. Cassidy, C. Chang, S. Gharib, and J. Torres. “Diagnostic Utility of Laboratory Tests in Septic Arthritis.” Emergency Medicine Journal24.2 (2007): 75-77. Web.